Knee
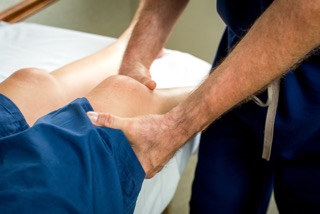
Anterior cruciate Ligament (ACL) Injuries
The anterior cruciate ligament, or ACL, is one of the major ligaments of the knee that is located in the middle of the knee and runs from the femur (thigh bone) to the tibia (shin bone). It prevents the tibia from sliding out in front of the femur. Together with posterior cruciate ligament (PCL) it provides rotational stability to the knee.
An ACL injury is a sports related injury that occur when the knee is forcefully twisted or hyperextended. An ACL tear usually occurs with an abrupt directional change with the foot fixed on the ground or when the deceleration force crosses the knee. Changing direction rapidly, stopping suddenly, slowing down while running, landing from a jump incorrectly, and direct contact or collision, such as a football tackle can also cause injury to the ACL.
When you injure your ACL, you might hear a “popping” sound and you may feel as though the knee has given out. Within the first two hours after injury, your knee will swell and you may have a buckling sensation in the knee during twisting movements.
Diagnosis of an ACL tear is made by knowing your symptoms, medical history, performing a physical examination of the knee, and performing other diagnostic tests such as X-rays, MRI scans, stress tests of the ligament, and arthroscopy.
Treatment options include both non-surgical and surgical methods. If the overall stability of the knee is intact, your doctor may recommend nonsurgical methods. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol); all assist in controlling pain and swelling. Physical therapy may be recommended to improve knee motion and strength. A knee brace may be needed to help immobilize your knee.
Young athletes involved in pivoting sports will most likely require surgery to safely return to sports. The usual surgery for an ACL tear is an ACL reconstruction which tightens your knee and restores its stability. Surgery to reconstruct an ACL is done with an arthroscope using small incisions. Your doctor will replace the torn ligament with a tissue graft that can be obtained from your knee (patellar tendon) or hamstring muscle. Following ACL reconstruction, a rehabilitation program is started to help you to resume a wider range of activities.
Meniscus Injuries
Meniscus tear or injury is the commonest knee injury in athletes, especially those involved in contact sports. A suddenly bend or twist in your knee cause the meniscus to tear. This is a traumatic meniscus tear. Elderly people are more prone to degenerative meniscal tears as the cartilage wears out and weakens with age. The two wedge-shape cartilage pieces present between the thighbone and the shinbone are called meniscus. They stabilize the knee joint and act as “shock absorbers”.
Torn meniscus causes pain, swelling, stiffness, catching or locking sensation in your knee making you unable to move your knee through its complete range of motion. Your orthopaedic surgeon will examine your knee, evaluate your symptoms, and medical history before suggesting a treatment plan. The treatment depends on the type, size and location of tear as well your age and activity level. If the tear is small with damage in only the outer edge of the meniscus, nonsurgical treatment may be sufficient. However, if the symptoms do not resolve with nonsurgical treatment, surgical treatment may be recommended.
Surgical Treatment
Knee arthroscopy is the commonly recommended surgical procedure for meniscal tears. The surgical treatment options include meniscus removal (meniscectomy), meniscus repair, and meniscus replacement. Surgery can be performed using arthroscopy where a tiny camera will be inserted through a tiny incision which enables the surgeon to view inside of your knee on a large screen and through other tiny incisions, surgery will be performed. During meniscectomy, small instruments called shavers or scissors may be used to remove the torn meniscus. In arthroscopic meniscus repair the torn meniscus will be pinned or sutured depending on the extent of tear.
Meniscus replacement or transplantation involves replacement of a torn cartilage with the cartilage obtained from a donor or a cultured patch obtained from laboratory. It is considered as a treatment option to relieve knee pain in patients who have undergone meniscectomy.
Cartilage Repair
Articular Cartilage is the white tissue lining the end of bones where these bones connect to form joints. Cartilage acts as cushioning material and helps in smooth gliding of bones during movement. An injury to the joint may damage this cartilage which cannot repair on its own. Cartilage can be damaged with increasing age, normal wear and tear, or trauma. Damaged cartilage cannot cushion the joints during movement and the joints may rub over each other causing severe pain and inflammation.
Cartilage restoration is a surgical procedure where orthopaedic surgeons stimulate the growth of new cartilage that restores the normal function. Arthritis condition can be delayed or prevented through this procedure.
Several techniques are employed for cartilage restoration including dietary supplements, microfracture, drilling, abrasion arthroplasty, osteochondral autograft, and allograft transplantation.
Dietary supplements: Dietary supplements such as glucosamine and chondroitin are the non-surgical treatment options for cartilage restoration. Chondroitin sulphate and glucosamine are naturally occurring substances in the body that prevent degradation of cartilage and promote formation of new cartilage. Chondroitin sulphate and glucosamine obtained from animal sources are available as over the counter products and are recommended for cartilage restoration. Apart from these various other nutritional supplements are also recommended such as calcium with magnesium and vitamin D as a combination, S-Adenosyl-Methionine and Methylsulfonylmethane.
Microfracture: In this method numerous holes are created in the injured joint surface using a sharp tool. This procedure stimulates healing response by creating new blood supply. Blood supply results in growth of new cartilage.
Drilling: In this method a drilling instrument is used to create holes in the injured joint surface. Drilling holes creates blood supply and stimulate growth of new cartilage. Although the method is similar to microfracture, it is less precise and the heat produced during drilling may damage other tissues.
Abrasion Arthroplasty: High speed metal-like object is used to remove the damaged cartilage. This procedure is performed using an arthroscope.
Osteochondral Autograft Transplantation: Healthy cartilage tissue (graft) is taken from the bone that bears less weight and is transferred to the injured joint place. This method is used for smaller cartilage defects.
Osteochondral Allograft Transplantation: A cartilage tissue (graft) is taken from a donor and transplanted to the site of the injury. Allograft technique is recommended if larger part of cartilage is damaged.
Autologous Chondrocyte implantation: In this method a piece of healthy cartilage from other site is removed using arthroscopic technique and is cultured in laboratory. Cultured cells form a larger patch which is then implanted in the damaged part by open surgery.
Osteoarticular transfer system (OATS): Osteoarticular transfer system (OATS) is a surgical procedure to treat isolated cartilage defects which usually 10 to 20 mm in size. The procedure involves transfer of cartilage plugs taken from the non-weight bearing areas of the joint and transferring into the damaged areas of the joint.
This procedure is not indicated for wide spread damage of cartilage as seen in osteoarthritis.
The procedure is usually performed using arthroscopy. During the procedure the plugs taken are usually larger and therefore only one or two plugs are needed to fill the area of cartilage damage. The area of damaged cartilage is prepared using a coring tool which makes a perfectly round hole in the bone in the area of damage. The hole is drilled to a size that fits the plug. Next the plug of normal cartilage is harvested from a non-weight bearing area of the knee, is then implanted into the hole that was created in the damaged area. The size of the plug used should be slightly larger than the hole so that it fits into the position. This procedure allows the newly implanted bone and cartilage to grow in the defected area.
Possible complications of OATS include donor site morbidity causing pain, avascular necrosis, and fracture. Other complications such as hemarthrosis, effusion and pain may also occur. Following OATS rehabilitation is recommended by use of crutches and limiting the range of motion.







