Shoulder
Labral Tears
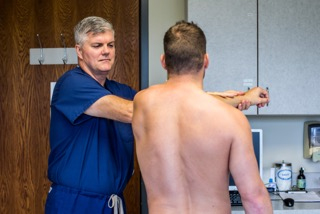
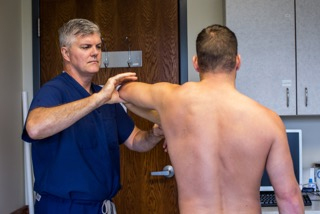
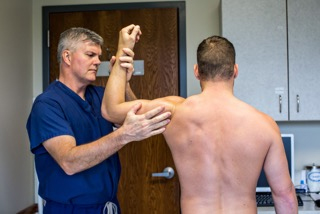
The shoulder joint is a “ball and socket” joint that enables the smooth gliding and thereby the movements of arms. However, it is inherently unstable because of the shallow socket. A soft rim of cartilage, the labrum lines the socket and deepens it so that it accommodates the head of the upper arm bone better.
Traumatic injury to the shoulder or overuse of shoulder (throwing, weightlifting) may cause labral tear. In addition, ageing may weaken the labrum leading to injury. Shoulder labral tear injury may cause symptoms such as pain, catching or locking sensation, decreased range of motion and joint instability.
Your doctor may start with conservative approaches such as prescribing anti-inflammatory medications and advice rest to relieve symptoms until diagnostic scans are done. Rehabilitation exercises may be recommended to strengthen rotator cuff muscles. If the symptoms do not resolve with these conservative measures, your doctor may recommend arthroscopic surgery.
During arthroscopic surgery, your surgeon examines the labrum and the biceps tendon. If the damage is confined to the labrum without involving the tendon, then the torn flap of the labrum will be removed. In cases where the tendon is also involved or if there is detachment of the tendon, absorbable wires or sutures will be used to repair and reattach the tendon. After the surgery, you will be given a shoulder sling to wear for 3-4 weeks. You will be advised motion and flexibility exercises after the sling is removed. These exercises increase the range of motion and flexibility of shoulder joint.
Shoulder Instability
Shoulder instability is a chronic condition that causes frequent dislocations of the shoulder joint.
Causes
A dislocation occurs when the end of the humerus (the ball portion) partially or completely dislocates from the glenoid (the socket portion) of the shoulder. A partial dislocation is referred to as a subluxation whereas a complete separation is referred to as a dislocation.
Risk Factors
The risk factors that increase the chances of developing shoulder instability include:
- Injury or trauma to the shoulder
- Falling on an outstretched hand
- Repetitive overhead sports such as baseball, swimming, volleyball, or weightlifting
- Loose shoulder ligaments or an enlarged capsule
Symptoms
The common symptoms of shoulder instability include pain with certain movements of the shoulder; popping or grinding sound may be heard or felt, swelling and bruising of the shoulder may be seen immediately following subluxation or dislocation. Visible deformity and loss of function of the shoulder occurs after subluxation or sensation changes such as numbness or even partial paralysis can occur below the dislocation as a result of pressure on nerves and blood vessels.
Conservative Treatment
The goal of conservative treatment for shoulder instability is to restore stability, strength, and full range of motion. Conservative treatment measures may include the following:
- Closed Reduction: Following a dislocation, your surgeon can often manipulate the shoulder joint, usually under anesthesia, realigning it into proper position. Surgery may be necessary to restore normal function depending on your situation
- Medications: Over the counter pain medications and NSAID’s can help reduce the pain and swelling. Steroidal injections may also be administered to decrease swelling
- Rest: Rest the injured shoulder and avoid activities that require overhead motion. A sling may be worn for 2 weeks to facilitate healing
- Ice: Ice packs should be applied to the affected area for 20 minutes every hour
Surgery
When the conservative treatment options fail to relieve shoulder instability, your surgeon may recommend shoulder stabilization surgery. Shoulder stabilization surgery is done to improve stability and function to the shoulder joint and prevent recurrent dislocations. It can be performed arthroscopically, depending on your particular situation, with much smaller incisions. Arthroscopy is a surgical procedure in which an arthroscope, a small flexible tube with a light and video camera at the end, is inserted into a joint to evaluate and treat of the condition. The benefits of arthroscopy compared to the alternative, open shoulder surgery are smaller incisions, minimal soft tissue trauma, less pain leading to faster recovery.
Rotator Cuff Tears
The rotator cuff is a group of tendons in the shoulder joint providing support and enabling a wider range of motion. Major injury to these tendons may result in a tear of these tendons and the condition is called rotator cuff tear. It is one of the most common causes of shoulder pain in middle aged adults and older individuals.
Causes
Rotator cuff tears result from pressure on the rotator cuff from part of the shoulder blade (scapula) as the arm is lifted. It may occur with repeated use of the arm for overhead activities, while playing sports or during motor accidents.
Symptoms
Rotator cuff tears cause severe pain, weakness of the arm, and a crackling sensation on moving the shoulder in certain positions. There may be stiffness, swelling, loss of movements, and tenderness in the front of the shoulder.
Diagnosis
Your surgeon diagnoses a rotator cuff tear based on the physical examination, X-rays, and imaging studies, such as MRI. Rotator cuff tears are best viewed on magnetic resonance imaging (MRI).
Conservative Treatment Options
- Rest
- Shoulder sling
- Pain medication injection consisting of a steroid (cortisone) and a local anesthetic in the subacromial space of the affected shoulder to help decrease inflammation and pain
- Specific exercises
Surgery
Rotator cuff repair may be performed by open surgery or an arthroscopic procedure. In an arthroscopy procedure, space for the rotator cuff tendons will be increased and the cuff tear is repaired using suture anchors. These anchor sutures help in attaching the tendons to the shoulder bone. Following the surgery, you may be advised to practice motion and strengthening exercises.







